Research review, and 'what is this guy up to' recap.
Thanks for reading the 52nd edition of my newsletter. This newsletter tracks my research as I write a book about sciatica, and another one (out very soon) about cauda equina syndrome.
By the way, if you’re not really enjoying these emails, you should unsubscribe! I hate the idea that they’re just clogging up someone’s inbox. Just scroll to the bottom and click ‘unsubscribe’ 👍
Hi from a rapidly heating-up Houston,
We are still holding fire with the CES book…
Why the wait? Well, there's new guidance coming out in the UK for CES. We don't want to put the book out and then find out that the guidance says something that conflicts horribly with what we've said. That's just going to cause problems for readers.
The thing is, we're pretty sure the guidance isn't going to say anything unexpected that clashes with the contents of the book. But we agreed that it's safest just to wait a bit to make absolutely sure...
So in the meantime I've been catching up with some of the sciatica literature. I thought I'd share the results from a few papers in this newsletter. But first…
A recap of what this newsletter is all about!
I wanted to take the time to recap what I'm actually doing with this newsletter and with all these books… I continually get new subscribers and I don't really do enough to let them know what it is they've subscribed to. So, if you’re interested in what I’m doing here, read this. If you’re not, skip it!
I started this newsletter in February 2020 with no particular goal other than to research sciatica and share my findings with others. A few editions in, I decided it would be good to write a book, mostly so that I had something to work towards. I had also just moved to the US (my wife is American), my work permit was delayed and covid had just kicked off... so the book was a way to keep working and earning, too.
After a while I realised what now seems obvious, which is that writing a book about 'sciatica' is far too big a task! So I split the book into two and focused on part 1, which was just about anatomy and pathology. I put that out as a pdf last year and people really liked it and it even made me some money. Great!
But working on the book was a bit of a lonely process, probably made worse by the fact that I had just moved to a new country, so I decided that rather than work on boko 2, I wanted to work on something with someone else. I contacted my friend and former mentor Rob and, some time later, we've finished that project, which is the upcoming CES book...
Oh, and in the meantime my daughter Hannah was born!
A few months ago I took the first sciatica book off the market. I want to improve it, improve the illustrations and publish it as a proper ebook and paperback rather than a pdf. That's what I'm going to do next. (If you bought the pdf, I will try to give a discount or something, to make sure that to get the improved version you don't have to 'buy the book twice').
Once that's done (dare I say, later this year) I will turn my eye to the second sciatica book on assessment and treatment. I have a lot of concerns about this because I don't think I have the breadth of experience and knowledge needed to write a really good book about such a broad topic. I don't think this is imposter syndrome, just a realistic appraisal of my strengths and weaknesses! My latest thinking is that I will try to find some coauthors or contributors for book 2, hopefully people who compensate for my weaknesses. We’ll see. At the end of the day the main goal is to make the book the best, most useful book it can be. I'm much more likely to do that with others’ help.
And this newsletter? It allows me to keep sharing what I’m learning. It helps to turn what could be a rather isolated and lonely process into a more social one. Also, writing things up as I go along helps me to stay rigorous, and subjects what I’m doing to feedback. And I’ve got to know a lot of great people through the newsletter.
So, I hope that helps some readers get a feel for what’s going on…
Okay, on to the research review.
💊 A qualitative exploration of patient experiences of medication for sciatica (Reddington, Baxter & Walters, 2021)
This study found that, when it comes to medications for sciatica:
People who are taking them don't think they’re working,
They're afraid of getting addicted,
They're hate the side effects and find them frightening ‘I was frightened of [amitriptyline] because they just made me feel drowsy and weird; you know, spaced out.’ ‘The whole of you just doesn't feel like you’, ‘[Tramadol] just messed me up and started me with panic attacks’.
And when meds didnt work, people stop taking them, and some start drinking alcohol or taking illegal drugs, from cannabis to heroin, instead.
Another notable thing is the sheer range of medications prescribed. Paracetemol, tramadol, naproxen, amitriptyline, co-codamol, ibuprofen, solpadol, gabapentin, diazepam, pregabalin, prednisolone, buprenorphine… No one really knows what, if anything, to give people with sciatica.
Oh, and how's this for a description of radicular pain: ‘It felt like someone had taken a knife and cut around the top of my leg and was peeling my skin down like you take off a stocking. It was burning all the way down’
🦵 A broad and variable lumbosacral myotome map uncovered by foraminal nerve root stimulation (London et al., 2022)
As long time readers know, the dermatomes are a lot more blurry, overlapping and random than the way they're depicted in textbooks. This study suggests the same is true for myotomes.
London and colleagues stimulated the nerve roots of patients who were undergoing surgery (the surgery was to implant a DRG electrode for CRPS). The authors found that:
L4 stimulation led to quad contraction, as expected, but only in 5 of 8 people... and it also contracted tib ant in 2 of 8.
L5 timulation led to tib ant contraction, as expected, but only in 8 of 12 people... and, it also contracted the quads in 4/12 and gastroc in 5/12.
S1 stimulation led to gastroc contraction as expected, but only in 12 of 26 people... and it contracted tib ant in 10/26 and abductor hallucis in 8/26
They also found that about a third of the time, one nerve root contracted muscles in two different myotomes. For example, L5 and S1 commonly innervated both tib ant and gastroc in the same person.
As with dermatomes and radicular pain patterns, it's not that the standard myotome charts are hopelessly wrong. As the authors say, 'the most observed actions were consistent with the known myotomes'. But there should be a big asterisk next to the charts in textbooks; 'I think you'll find it's a bit more complicated than that...'
🐭 Effect of Physiotherapeutic Interventions on Biomarkers of Neuropathic Pain: A Systematic Review of Preclinical Literature (Matesanz-Garcia et al. 2021)
You wouldn't believe how much research there is testing physiotherapy treatment for nerve injuries in rodents. There's oodles of it. Little mice getting neurodynamic mobilisations and little rats on treadmills. I’ve often wondered what to make of it all. Luckily this paper by Matesanz-Garcia, along with Annina Schmid, explains the main findings.
The good news is that exercise seems to be good for injured nerves. It reduces pro-nocieptive markers markers in nerve tissue (think 'scary sounding acronyms': NGF, TRPV1, CD68, BDNF...), and increases anti-neuropathic markers (e.g. opiods). Swimming, treadmill training, whatever.
In one respect, this is expected because we know that exercise reduces inflammation.
In another respect, it's unexpected because these rodents had nerve injuries, often traumatic ones, and it's not obvious that running and swimming (sometimes to exhaustion!) wouldn't just make those injuries worse.
I remember saying this to David Butler during our podcast: while it feels imtuitive that exercise is good for muscle injuries, it's harder to feel really comfortable with the idea of exercising an injured nerve. It's partly cultural I suppose, we just feel like nerves are delicate little things. So this paper, to me, is another little bit of evidence to support what the researcher Giacomo Carta told me about exercising painful and injured nerves: it's safe!
So, with the usual caveats about animal studies, this study is another little weight on the scale in favour of the conclusion that, for people with nerve injuries, tolerable exercise is generally safe and probably makes nerves healthier.
🔪 Outcomes After Lumbar Disk Herniation Surgery in the Dutch Population (Schepens et al., 2021)
A huge study that included data from 6,895 people in the Netherlands who had an operation for a herniated disc between 2015 and 2016. The authors got their data from an insurance claims database. As far as I can tell, this is a fairly representative sample. The key points:
Within one year of their op:
5.6% of people had had a re-operation.
6.7% of patients had had a nerve root injection.
16% of people were using opioids (although it was not possible to determine from the database if the opiods were for their sciatica)
23% of people had at least one of the outcomes mentioned. You have to assume that some people also had a bad outcome that didn't include the three things—re-op, injection, opioids—that the study looked for, and that therefore the true number of bad outcomes is higher.
I don't know the literature well enough to say how representative this study is. Working on it!
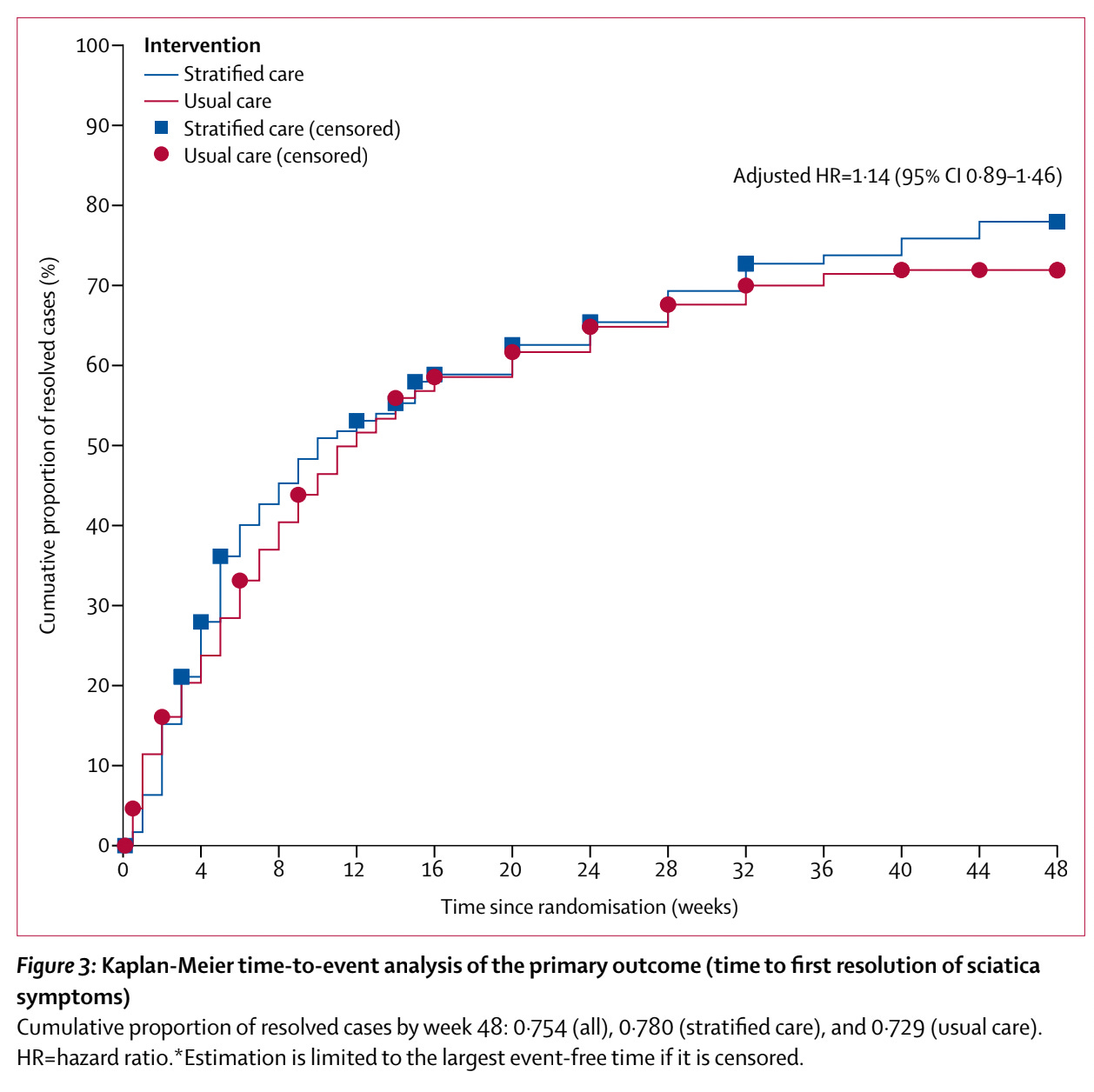
🪜 Stratified care versus usual care for management of patients presenting with sciatica in primary care (SCOPiC): a randomised controlled trial (Konstantinou et al., 2020)
This trial aimed to compare 'stepped care' to 'stratified care' for people with sciatica.
Stepped care is what we usually see: start with the most conservative option and if that doesn't work, 'step' up from there to things like imaging, specialist assessment, injections and finally surgery. Stratified care, on the other hand, is where you try to anticipate what level of care patient will need from the start, based on their symptoms. If you use Keele STarT Back to help you decide where to point patients, that's stratified care.
If we could stratify care that would be great, because then we wouldn't have to make patients endure ineffective treatment before we try something that might work better.
Unfortunately, this trial found that the stratified care goal is some way off for people with sciatica. The results between the stratified care group and the usual (stepped) care group were practically identical.
Here's a bit more detail. The authors stratified patients by clinical features: leg pain, pain below the knee, interference with activities and neuro loss. Patients with the mildest symptoms were put in the lower strata and given two sessions of physio with a self-management angle. Patients with middling symptoms were put in the middle strata and offered up to six sessions of physio. Those in the highest strata had, you guessed it, the worst symptoms, and were fast-tracked to MRI and a spinal specialist.
In all, 238 patients were stratified, and their outcomes were compared to 238 patients in usual care. The authors had a nice and simple, meaningful outcome measure: time to recovery of sciatica.
The clinical course of the two groups looked like this:
What explains the lack of difference between the groups?
Maybe it's because stratification is just hard in the real world. For example, the diagnosis of 'sciatica' probably meant the patients were a mixed bag (at the very least they weren’t ‘raging radicular pain’ patients; some didn’t have a positive straight leg raise and most had no loss of strength). Surely waiting times, missed appointments etc. had their part to play. The authors also note that some clinicians were reluctant to use the fast track for some patients. (None of this is a criticism of the authors, it's all just the nature of pragmatic trials). Maybe if things like that could be ironed out, stratification would work.
On the other hand, maybe there's no difference between stepped and stratified care because there aren't really any hugely effective treatments to stratify to. Are six sessions of physio that much better than two? And are six sessions of physio really worse than an an appointment with a specialist who might refer for an injection or operation? The pessimist would say that, like many conditions, most of the clinical course of sciatica is just natural history, and stratification is unlikely to change that…
As usual, it’s probably a bit of both.
In any case, this study also provides some of the best data on the clinical course of sciatica. Patients had a mixture of very acute and chronic sciatica, but about three quarters had had pain for less than twelve weeks, so as a group they tended towards a more recent onset. Here’s how they did:
After 3 months, half of patients said their leg and back symptoms were either ‘completely recovered’ or ‘much better’.
After a year, this number was three quarters. (Glass half empty: after a year, one quarter were still struggling…)
🏥 Surgery versus Conservative Care for Persistent Sciatica Lasting 4 to 12 Months (Bailey et al. 2020)
Last study. It's generally accepted that surgery for sciatica works, to an extent. But almost all the evidence studies people who have had sciatica for less than three months. So people often wonder: does surgery still work for people with chronic symptoms?
In this study, it did.
(Note that the results are also a reminder that surgery for radicular pain also improves the back pain!)
Of course, the fact that surgery works on average doesn't mean it's worth it for any one patient. What about the adverse events? There were eleven of them, in nine patients, out of 78 people who had surgery. These included one dural tear, one nerve root injury, two wound infections and two re-herniations... Worth it the risk for a mean 2.4 points difference in pain at six months?
And that’s it for this week…
There you have it. I quite enjoyed catching up with some of the literature.
That said, it’s a bit dispiriting sometimes that there are never many (or really any) papers that say ‘hey this great new thing works really well!’
But that motivates me. When the research landscape has no outstanding treatments and few conclusions, and the clinical landscape is also very varied and uncertain, a book to help clinicians to navigate that landscape is all the more needed.
Til next time,
Tom