*That* nylon thread study
(Journal club 2)
Hi everyone,
Here's an unforgettable experimental study. It's firmly in the annals of 'you couldn't do that these days'.
The study was performed at St James's Hospital in Leeds in 1958. At the time, people knew that disc herniations are a principal cause of sciatica. But they didn’t really know anything about how those herniations caused pain. Most people thought that it was through pressure: discs put pressure on nerve roots and that pressure causes pain, sort of like a poke in the eye. But the authors of this paper, Doctors Smyth and Wright, had a hunch that it wasn't quite that simple.
Here's what Smyth and Wright did. They took 40 of their patients with 'sciatica' (i.e. radicular pain +/- radiculopathy) due to a herniated disc. As usual, they operated on these patients to remove the herniated disc material. Then, once the material was removed, they took a nylon thread and looped it round the involved nerve root, bringing both ends of the thread to the surface. They sewed and patched their patients up, leaving the ends of the thread hanging out.
They waited a few days for their patients' pain to resolve post-op...
...Then, they pulled on the nylon thread.
Only gently, you understand. In their words, 'just a gentle pull was exerted to bring the nylon in contact with the root, causing a moderate degree of pressure'.
What happened? Here's how Smyth and Wright describe Case 1, a participant with the initials R.S. who had an S1 radiculopathy:
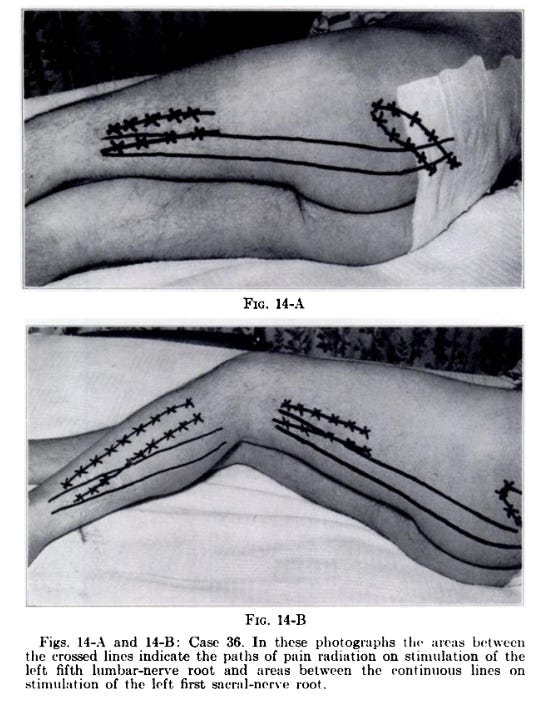
'The effect [of a gentle pull on the thread] was immediate. The patient jumped and exclaimed that a severe pain shot into the right buttock. It disappeared at once when the nylon was relaxed. At the second attempt the thread was very slowly drawn upon until the patient could feel pain. This time it was not so intense: the thread could be barely touching the root. Then tension was increased and as it mounted severe pain spread from the center of the right buttock down the center of the back of the right thigh, veered laterally to the region of the biceps tendon, skipped the side of the knee, and was felt intensely on the lateral side of the calf. It ended about three inches above the lateral malleolus. [The pain] appeared to consist of two components: a sharp pain which ran, as if along a line, down the extremity, and a deep, boring, aching, unpleasant sensation felt diffusely in the soft tissue'.
Next, they pulled on the thread in the same manner, but this time looking out for changes in sensation. Here's what happened: 'After a continuous but gentle pull for a quarter of a minute, the patient volunteered the information that all of the toes and part of the dorsum of the foot, proximally, felt numb'.
Their work done, Smyth and Wright pulled out the thread and closed the wound.
In Case 2, a patient with the initials J.S., 'an almost identical series of events occurred'. And the same happened in the next case, and the next. In almost all cases, a gentle pull on the nylon thread around the involved nerve root brought about 'a series of events similar in every way': a perfect, instant, severe reproduction of that patient's pre-op pain. And, less frequently, with a prolonged pull, there was also sometimes the same numbness.
The authors also noticed that they could change how far the radicular pain spread down some patients' legs by changing the amount of force they used to pull on the thread. A particularly gentle pull would cause proximal radicular pain, and slowly adding pressure would cause the pain to expand distally. As they put it, 'the longitudinal spread of the pain was proportional to the degree of increasing pressure... it only spread further when the pressure was increased.'
This is a good time to talk about the ethics of this paper... The sheer chutzpah of this experiment is what makes the paper stand out, but since this is a time before ethical review boards there is the disquieting concern that Smyth and Wright were abusing their position of power. For what it's worth, here is their explanation: 'There was no suffering for the patients. The purpose of the experiment was explained to them and they all took a cooperative and intelligent part in the proceedings. Indeed some asked to have the root stimulated repeatedly so that they could more accurately localize the pain. Nevertheless, it could not be described as an enjoyable performance'. I’ll bet…
On with the paper. With some of their 40 patients, Smyth and Wright made additions to their experiment. In five, they passed an additional loop of thread through the dura mater of the dural sac (the dural sac, sometimes called the thecal sac, is the cover of the main bundle of the cauda equina; see this 'tour' if you're not too familiar with lumbar anatomy!).
What happened when they pulled the thread around the dural sac? In three patients, not much; the dural sac was either insensitive or virtually insensitive. In two patients, there was an aching pain, one in the back and one in the buttock. In no patients did pulling on the dural sac cause anything like radicular pain.
In six patients, as another addition to their experiment, Smyth and Wright passed an additional loop around the neighbouring, uninvolved nerve root. For example, if the involved root was S1, then they passed a loop around S1 but also L5 as well.
What happened when they pulled on the thread around the neighbouring, uninvolved nerve root? This too caused some radicular-ish pain. The distribution of this pain was very close to and in some cases overlapped with the pain caused by pulling on the involved nerve root.
Crucially, the pain caused by tugging on the thread around an uninvolved, uninjured root was much less severe than the pain caused by stimulating an injured root. As Smyth and Wright put it:
'The nerve root which had been pressed upon by a disc was much more sensitive to the touch of the thread than a neighbouring nerve root which was not involved in the herniation. Prolonged irritation appeared to have made the root hypersensitive.'
In 11 patients, Smyth and Wright didn't test the roots but the surrounding tissues: ligamentum flavum, interspinous ligament and annulus fibrosus. For some patients, pulling on these tissues caused no sensation at all. For some, it caused a dull ache, or a dragging sensation, usually around the spine but in one case in the back of the knee. According to the authors, these aches and dragging sensations 'could scarcely be described as pain'. They were sometimes slow to arrive after stimulation, and sometimes lingered after stimulation had stopped.
This paper is a gold mine of interesting observations. Like last fortnight's paper, it's old enough that the authors are unconstrained by modern formalism and are unafraid to simply say what they see. I recommend reading the entire thing to hear about Smyth and Wright's descriptions of the herniations and adhesions they saw, the pain patterns their patients described, and other tidbits (for example, they found that in some patients, repeatedly pulling on roots caused initially severe pain to subside over time... McKenzie centralisation?).
So rather than list every single thing in this paper, I will just focus on one of the key messages as I see it.
That is that radicular pain doesn't necessarily mean a nerve root is being pressed, squashed or crushed. Smyth and Wright reproduced their patients' radicular pain precisely, using just 'a gentle pull'. By contrast, the same amount of pressure on a neighbouring, unaffected nerve root didn't cause symptoms anything like as severe. On top of that, Smyth and Wright noticed that some of the herniations they removed were very small indeed, and couldn’t have been putting much, if any pressure on the injured nerve roots.
This has clear historical significance. It helped to counter the prevailing structuralist assumption that nerve root pain was just about pressure. Now, thanks to research performed since Smyth and Wright, we understand that there is a missing piece to that assumptions, which is inflammation, triggered by the herniation (more here).
To put it another way, in many cases radicular pain might be less analogous to a finger poking you in the eye, and more analogous to a finger touching you lightly in the eye, but that finger is covered in chilli powder...
However, Smyth and Wright's finding also has relevance to our patients. It is potentially reassuring. In my experience, a lot of people with radicular pain assume that every time they get a jolt of pain it’s because their nerve root is being squashed by a 'slipped disc'. It's a very mechanical picture that can't be very nice to imagine. Bend —> squash —> ouch.
However, and again this is just my experience, a lot of people feel reassured to know that it's quite likely that this is not the case. Instead, it's quite probable that their nerve root is just very sensitive, and moving it and stretching it just hurts full stop. Now, this isn't going to have patients dancing out the door, but many people are relieved to hear that pain with movement doesn’t necessarily mean they’re squashing the nerve root, and find it gives them the confidence to move a bit more.
That said, we have to be careful with this message because of course some people do have large disc herniations that mechanically squash or crush their nerve roots. In fact, another interesting thing about this paper is that although in some ways it undermines a purely structuralist explanation of radicular pain, in other ways it confirms how very important peripheral structures are to the clinical picture of radicular pain. It demonstrates a predictable cause --> effect relationship between disc herniations, injured nerve roots and radicular pain. It's just that we have this added factor of the roots being enduringly sensitised by inflammation.
Well, that’s it for now. I hope this was insightful. If you read this paper (link here) I’d be curious to hear what you found interesting!
Til next time,
Tom
P.S. I just wanted to show off some pictures that people have been posting online of their copy of Cauda Equina Syndrome: The Clinician’s Guide. To read reviews and find if the book is right for you click here:
…And I’m afraid I will continue to plug it for the next couple of weeks. Gotta be done!